
Anyone going through the undeniably stressful experience of IVF is bound to be familiar with all sorts of jargon associated with embryo development and how embryos are graded. After getting through each stage of the IVF process, from testing and diagnosis to egg collection and fertilisation, it is incredibly disappointing to hear that your embryos are of poor quality. But there is always hope, and plenty of IVF success stories about embryos that have achieved dreams in the face of the extraordinary circumstances.
Despite technological advances in embryo evaluation, embryo grading remains an art based on embryologists’ years of experience rather than a strictly exact science. Many women and couples have had the thrill of good news after a less-than-promising prognosis. Even for women with a low ovarian reserve, IVF success rates can be excellent, and even poor-quality embryos can end up with a heart-warming success story.
What is a poor-quality embryo?
After the fertilisation of eggs in the laboratory, embryologists study embryos as they develop. They are graded and selected for transfer back to the womb at either Day 3 or Day 5 of development, each with different criteria and grading ‘scores’.
Cleavage-stage embryos
Day 3 embryos are known as cleavage-stage embryos. The cells have started to divide, or ‘cleave’, but the embryo is not yet growing; it remains the same size as the mature egg that has been fertilised. The number of cells present is one of the criteria by which cleavage-stage embryos are graded. The other is the appearance of the cells and whether there is any fragmentation (where a portion of the cell’s cytoplasm breaks off into a fragment).
Grading is on a scale of 1 to 4, with 1 being good quality and 4 being poor. Typically, a grade 1 cleavage embryo would have at least 6 cells of equal size and no fragmentation. Grade 4 could have cells of equal or unequal size, with moderate to heavy fragmentation.
Blastocyst stage embryos
In the UK, the majority of IVF transfers (75%) are carried out on Day 5, at the blastocyst stage, so the way these are graded is likely to be familiar to more people undergoing IVF. In the blastocyst stage, cells have continued to divide, and there are now 100 to 125 cells. They are also growing and differentiating into different types of cells. The two types are the Inner Cell Mass (ICM), which will develop into the foetus, and the Trophectoderm Epithelium (TE), which will become the placenta. Both are essential to a successful pregnancy. Embryos are graded on both on a scale of A to C. Each grade is preceded by a number representing the expansion of the embryo cavity on a scale of 1 (poor) to 6 (good).
The ‘best’ grade would therefore be 6AA; a poor-quality embryo could be 4CD. However, it’s important to remember that embryos can change their ‘score’ as they develop and that while the chances of a successful pregnancy from a poor-quality embryo are lower, there is still a real chance.
A 2019 study, analysing over 900 euploid embryos, offers us the following data:
| Grading | Example Grade | Live Birth Rate |
| Excellent | 3AA, 4AA, 5AA, 6AA | 50% |
| Good | 3AB, 5AB, 3BA, 5BA, 4AB, 6AB | 49.7% |
| Average | 3BB, 4BB, 5BB, 6BB | 42.3% |
| Poor | 4BC, 6BC, 5CB, 5BC, 4CB, 6CB | 25% |
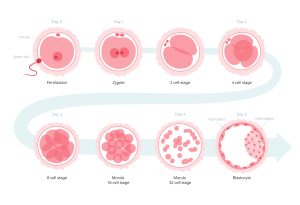
Embryonic development by day
Poor-quality embryo success stories
Leaving the technicalities behind, we are happy to share poor-quality embryo success stories from patients who have achieved their dream of becoming a parent despite a lower-grade embryo.
Caroline
Caroline and her husband had unexplained infertility. They had three unsuccessful attempts with IUI treatment before trying IVF. She ended up with 14 embryos but was concerned because of her age (37) that they may have an abnormality and so she requested genetic testing. Genetic testing returned 6 healthy embryos. The first transfer, graded 4AB, failed. The second and third, graded 6BA and 4BB, also failed. The following two transfers, graded 4BB, were unsuccessful. The final transfer took place: an embryo that was slow to develop, graded 4BB on Day 7 of development. The embryologist warned her not to be too hopeful, as the frozen embryo was downgraded to 4BC after thawing. Sure enough, there was a phone call to say ‘Congratulations’! Caroline and her husband have just celebrated the birth of their first child.
Elena
Elena also had unexplained infertility. After 3 separate egg collections resulting in unsuccessful implantation, even though the embryos were graded 5AA, she had almost given up. On her final egg retrieval, 10 mature eggs were whittled down to 3 embryos which developed to the blastocyst stage. The first, graded 5BB, did not implant, nor did the second, graded 3BB. Finally, the transfer of her last embryo, graded 3CC, led to success, and she is now the mother of a happy and healthy baby boy.
Maria
Maria, having been diagnosed with early onset menopause at the age of only 36, was devastated when she was advised to try IVF with donor eggs because her ovarian reserve was so low. She consulted a different clinic, which advised her to try IVF with her own eggs but with a carefully individualised medication protocol. She was amazed and delighted when her egg retrieval resulted in 6 eggs, 3 of which were fertilised and made it to the blastocyst stage. All three were frozen and, on two subsequent transfers, resulted in successful pregnancies.
Find out more about IVI
If you’d like to know more about IVI, or talk to a specialist about your personal chances of successful fertility treatment, even with adverse conditions like a low ovarian reserve, do get in touch.








Comments are closed here.