

Intracytoplasmic Sperm Injection (ICSI) is a procedure which can be used as part of IVF treatment. It takes place within the laboratory and involves an embryologist individually selecting the optimal sperm and injecting directly into an egg to facilitate fertilisation. It's often recommended for couples and men experiencing male factor fertility issues.


Intracytoplasmic Sperm Injection (ICSI) is a laboratory procedure which can be used as part of IVF treatment. It is designed to help couples who are experiencing male factor infertility issues. The procedure involves an embryologist individually selecting optimal sperm to be used and injected directly into an egg to facilitate fertilisation.
Your consultant may recommend adding ICSI to an IVF treatment in the following cases:
RESULTS
Over the last 30 years, IVI has helped more than 250,000 dreams come true.
CARE
97% of our patients recommend IVI. We’re with you at every stage of your treatment, providing support and care.
TECHNOLOGY
IVI has a worldwide reputation for innovative research and has developed and patented pioneering techniques and technologies.
EXPERTISE
IVI is one of the largest fertility treatment providers in the world, with more than 75 clinics in 9 countries.
Before starting the treatment pathway, you’ll have an initial consultation and scan, along with any necessary consent and screening. During this stage, your consultant will outline your personalised plan and prescribe fertility medicines to support ovarian stimulation. You’ll also receive clear instructions on when to take your trigger injection, and the timing of your egg collection and sperm production will be coordinated accordingly. If required, surgical sperm retrieval may also be arranged as part of this preparation.
If it is recommended that you undergo an in vitro fertilisation (IVF) treatment with ICSI, then we will create a treatment pathway for you, which is as follows:

In a normal menstrual cycle, a woman grows a single follicle, producing a single egg (oocyte), each month. During IVF, the ovaries are stimulated to grow more follicles, producing more eggs. The aim of this is so that when the eggs are collected, there will be a higher cumulative chance of successful fertilisation within the laboratory and a higher chance of developing multiple good quality embryos that can be transferred back into the uterus.

Depending on the chosen stimulation protocol, the stimulation process should take between 10 – 20 days and will require regular visits to the clinic. During this time, you may also be required to take specific medication to help prepare your body for the IVF treatment. Your medical team will indicate which medication is needed and the recommended dosage based on your unique requirements. This often involves a series of daily hormone injections, which are administered at home, to stimulate follicle growth. We track the follicle growth through frequent monitoring ultrasound scans and blood tests to assess serum levels in the blood.


When the follicles have reached an adequate size and number, it is time to schedule the oocyte retrieval procedure, known as an egg collection. The procedure will be timed to take place around 36 hours after an hCG injection is administered, which induces oocyte maturation and triggers ovulation. Your hCG injection is administered at home. Your medical team will provide clear and thorough instructions on how, and when, to administer your hCG injection. The egg collection takes place in the clinic under sedation and lasts approximately 15 minutes. You will need to stay in the clinic for at least a couple of hours to recover from sedation.
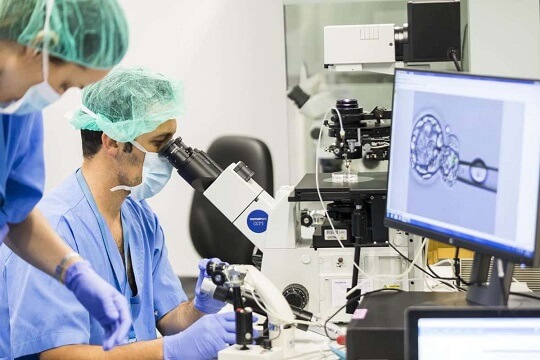
Before the ICSI procedure takes place, embryologists examine and select the sperm with the best motility and morphology. A single sperm is then injected directly into the egg using a micropipette to facilitate fertilisation. This differs to conventional IVF, in which semen is mixed with an egg and left to fertilise. After this stage, the IVF treatment resumes as normal and the resulting embryos are allowed to develop for 5 days in the laboratory before being transferred into the uterus.



The fertilised eggs are closely monitored in the laboratory as they begin to develop into embryos. In the following days, our embryologists will be able to grade the embryos based on their embryonic development, according to their morphology and ability to divide. Some embryos can become blocked in their development and will not be able to be transferred back into the uterus, as they will be considered non-viable.
An embryo transfer procedure involves placing an embryo into the uterus using a narrow catheter. The procedure is simple, quick and painless and is carried out in the clinic. At IVI, we follow a strict Single Embryo Transfer (SET) policy for the safety of both mother and baby. If you have a good quality embryos, choosing to transfer more than one embryo does not increase the chances of becoming pregnant, only the chances of having a multiple pregnancy and its associated risks.



In some cases, there are extra embryos remaining after an IVF procedure has taken place. Good quality embryos can be vitrified and preserved for a later cycle, removing the need to undergo ovarian stimulation and another egg collection.
ICSI (Intracytoplasmic Sperm Injection) is one of several types of assisted reproductive technology (ART) used to help individuals and couples conceive. It is often recommended in cases of male factor infertility, particularly when sperm count, motility, or morphology is significantly reduced.
ICSI treatment is a significant investment, and it’s essential to understand the associated costs before embarking on your journey. The total cost will depend on your personalised treatment plan and any additional procedures required.
We’re committed to making treatment as accessible as possible, with transparent pricing and a range of payment and financing options to support you.
You can view our full price list here.
While IVF (In Vitro Fertilisation) involves mixing eggs with sperm in a lab dish and allowing fertilisation to occur naturally, ICSI takes it a step further. A single, healthy sperm is selected and microinjected directly into the egg. This laboratory technique is especially useful when sperm quality is low or when previous IVF cycles have failed.
IUI (Intrauterine Insemination), on the other hand, is a much less complex procedure. Sperm is inserted directly into the uterus during ovulation, but fertilisation still occurs inside the body. IUI is usually only suitable for cases where sperm function is relatively normal.
We are proud to offer some of the highest live birth rates among private clinics in the UK. All of these can be found on our success rates page for different age ranges and treatment types. One common theme that exists is that we exceed the UK national average across all categories. Our success is based on personalised care, cutting-edge technology, and years of experience in infertility treatments. Each patient’s situation is unique, which is why we recommend a full consultation with one of our fertility experts to understand your individual chances of achieving a successful pregnancy.
We understand that fertility treatment can be both physically and emotionally demanding. That’s why our patient support team is here to guide you through every step. We also offer access to infertility counsellors, and clear communication with our fertility specialists at all times.
From your initial semen analysis and consultation to your final treatment steps, we’re committed to making your experience as informed and supported as possible.
Yes. ICSI is commonly used in conjunction with surgical sperm retrieval techniques such as PESA (Percutaneous Epididymal Sperm Aspiration) and TESE (Testicular Sperm Extraction), especially when sperm cannot be obtained naturally. Experienced fertility specialists perform these procedures to support patients with azoospermia or other sperm-related issues.